Pressure Ulcers
What is a pressure ulcer?
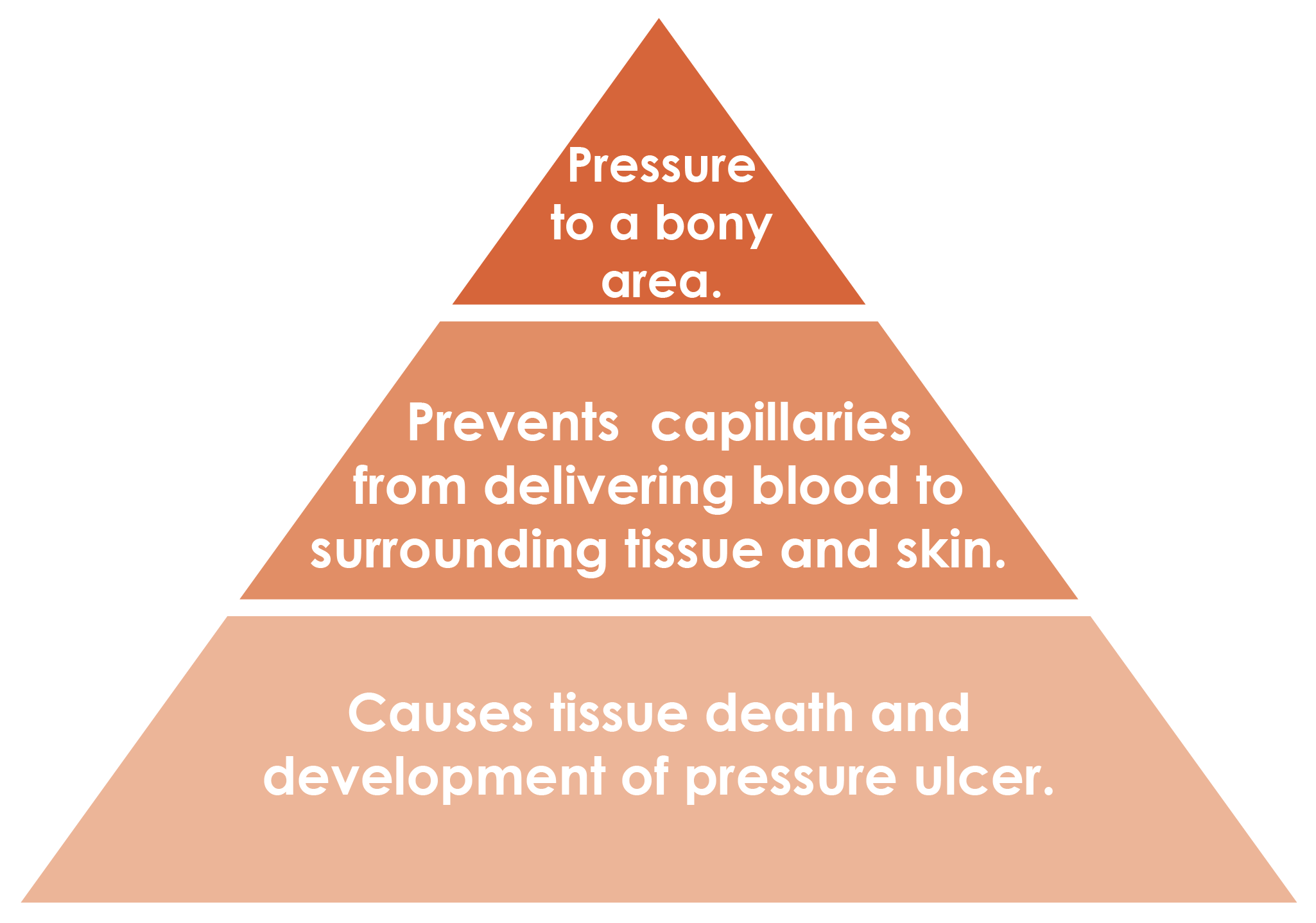
A pressure ulcer is:
- Damage to the skin and the deeper layer of tissue under the skin.
- They usually occur over a bony prominence and can be caused by a medical or other device such as casts, braces or anti-embolism stockings.
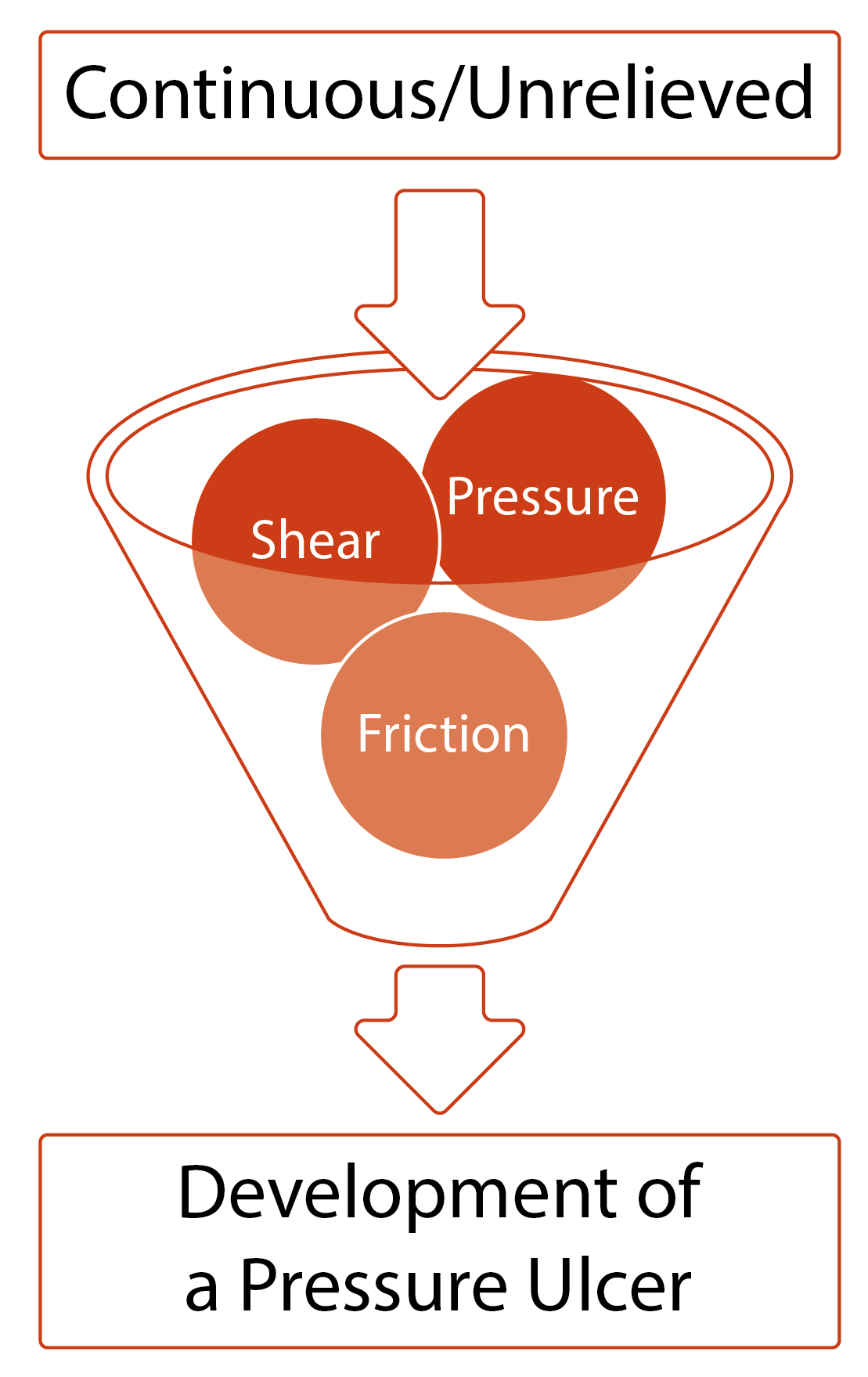
- They develop due to pressure, shear and friction.
- They can present as intact skin or an open ulcer and may be painful.
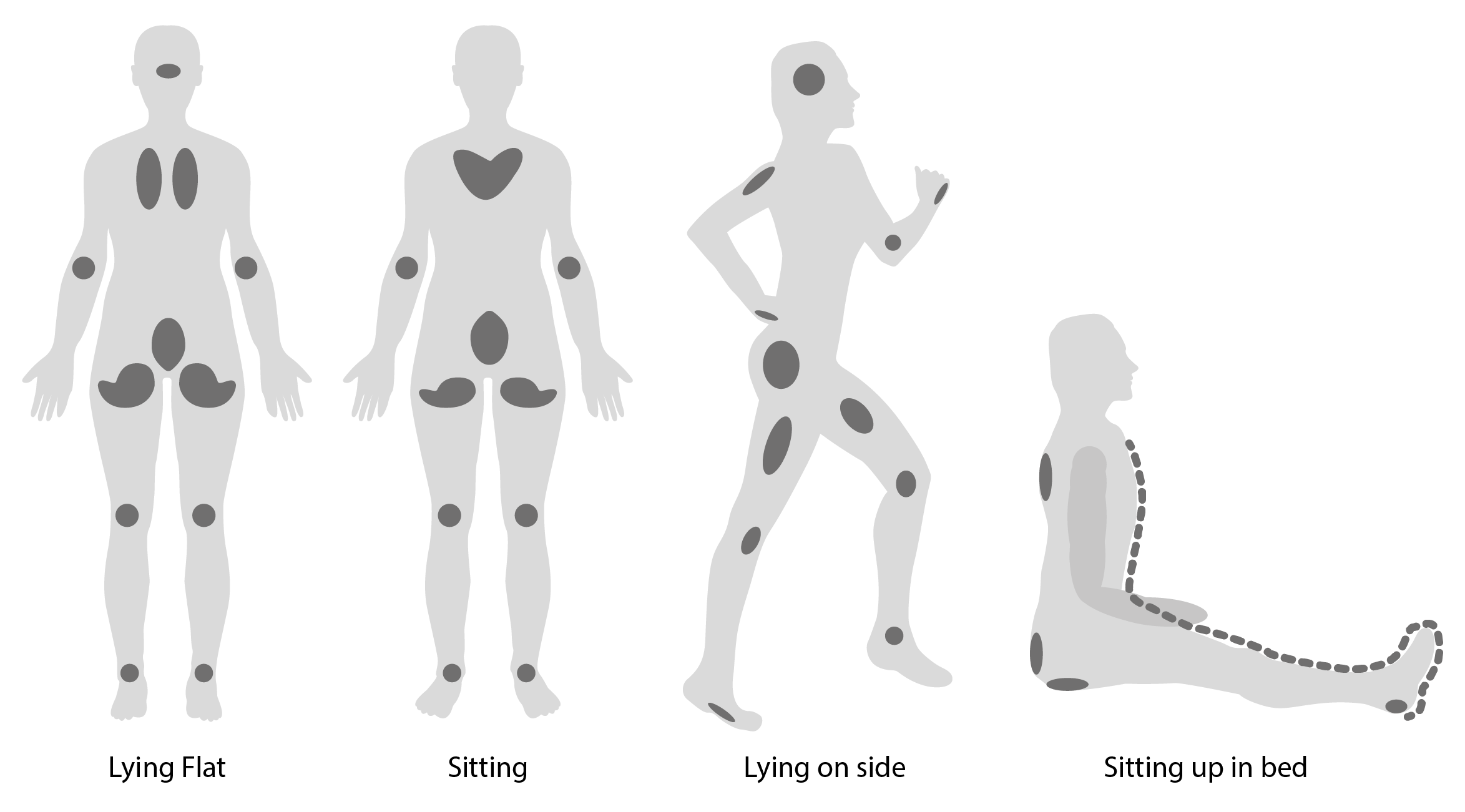
Where do pressure ulcers occur?
Pressure ulcers can affect any part of the body that's put under pressure. They're most common on bony parts of the body, such as the heels, elbows, hips and base of the spine.

Can pressure ulcers be prevented?
Yes, most pressure ulcers can be prevented by following these principles:
- Relieving pressure by moving, standing or turning regularly.
- Eating a balanced diet and drinking at least 6-8 glasses of water per day.
- Observing skin and reporting any redness or purple areas (that may look like a bruise) to your healthcare professional.
How can we help you?
The Tissue Viability team within the hospital has developed a strategy for all patients that have persistent red skin or discoloured skin called “Think Skin, React to Risk’. This pathway is aimed to help identify patients who are at high risk before they begin to develop signs of pressure damage. If commenced on this pathway you will notice the logo above the bed.
How can you help yourself?
- Eat and sleep well
- Try not to sit in one position for longer than an hour
- Move yourself on the chair
- Stand up and go for a walk if you can
- Lift your heels off the bed
The most important thing is to move around at least every 30 - 60 minutes. Please don’t worry we want to help you prevent pressure damage.
Who is at risk of developing pressure ulcers?
Everyone is at risk of developing pressure ulcers; no one is immune. However, they are more common in those who are very young or very old due to the nature of their skin. Other risk factors include those who:
- Cannot move easily
- Cannot feel/perceive pain
- Are incontinent
- Are acutely unwell or been for surgery
- Have a poor diet and may be dehydrated/suffering with dry mouth
- Have either an injury or illness where they cannot feel their lower limbs e.g Spinal Injury, MS.
- Are suffering with long COVID.
Useful contact numbers
- Main hospital number - 0121 685 4000
- Pre-Operative Assessment Clinic - 0121 812 3323
- Tissue Viability - 0121 812 3464
- Discharge Liaison Sister - 0121 812 3902
- Patient Advice and Liaison- 0121 812 3555
- You can also contact the ward you have been discharged from.