
Posterior Correction
What is scoliosis?
A scoliosis is a three-dimensional curvature of the spine (back bones). A scoliosis can develop for a number of reasons and varies enormously in severity between individuals. There are many different types of scoliosis based on age and the type of curve. A curve can develop at any part of the spine and can be either a single or multiple curves resulting in a ‘C’ or ‘S’ shape when looking from behind.
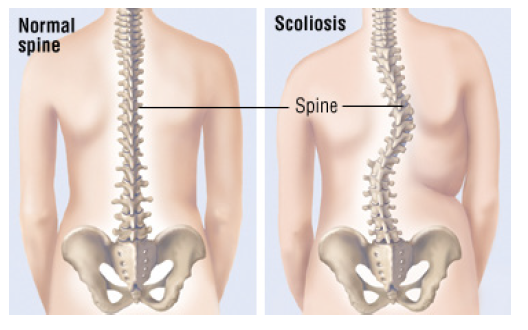
Why am I having surgery?
Surgery is only indicated in scoliosis when your curve becomes more severe, or it has a significant effect on your day-to-day functioning. There are several different types of operation that can be considered to correct your curve, and these will be discussed with you by your consultant.
What happens during surgery?
During your corrective surgery your surgeon will make an incision (cut) through the skin and muscles over your back. Your consultant will then straighten your spine as much as it is safely possible to do so and a series of metal rods, screws and hooks will be inserted to hold the correction whilst a bony fusion occurs. This metal works stays in unless there is a problem in future.
What should I expect after my surgery?
Mobilisation
You will be seen by the physiotherapists the day after your surgery. They will check that your legs are working normally following your surgery and that your chest (breathing) is okay. You will be allowed to start sitting up and standing with the assistance of the physiotherapists the day after your surgery. You will be shown how to safely get in and out of bed by ‘log-rolling’ to protect your spine and you will be assisted to start walking and sitting out in a chair you will be encouraged to walk regularly throughout the day. By the time you go home you will be walking around the ward on your own. You will also be shown how to get up and down stairs safely, if this is required.
Breathing exercises
Due to the length of your anaesthetic and the location of surgery you will be required to complete breathing exercises. This is to make sure that you do not develop any complications with your chest such as infections. You will need to complete these exercises regularly whilst you are in hospital and once you go home.
Other exercises
You will not be given any specific exercises for your back as it is essential that the bones heal properly. You are advised not to complete any form of bending, lifting or twisting for 6 weeks after your surgery. After this time, you will be guided by your consultant. At home it is important that you gradually increase how much you are walking around, continue with your breathing and arm exercises and complete any postural advice that you may have been given by your physiotherapist on the ward. You should be reviewed by your consultant at six weeks post operation. If you require additional physiotherapy this will be considered at around six months post-operation.
Caring for yourself
It is important that you start to complete your normal daily routine as soon as possible after your surgery. It is expected that you will need some assistance from the nursing staff to begin with however by the time you go home you should be able to get in/out of bed and care for yourself as you would normally do so. You may be assessed by the occupational Therapist for any additional equipment that you may need to make things easier at home.
Pain relief
You will normally have an epidural and PCA (patient-controlled analgesia) for pain relief after your surgery. The epidural can make parts of your legs feel a bit numb after your operation. These will be stopped at around 24-48 hours after your surgery and you will be given oral medications to take instead. Due to the nature of your surgery, it is expected that you will experience some pain afterwards. It is important to take these as prescribed to keep pain to a minimum and allow you to mobilise.
Bladder and Bowels
You will have a catheter inserted whilst you are asleep to allow us to monitor your urine output over the first few days after your surgery. This will be removed at the earliest opportunity.
Due to the combination of strong opioid painkillers, a long anaesthetic and reduced mobility you will become constipated. You will be given regular laxatives to help with this but may need more invasive assistance such as suppository or an enema.
Wound care
If you develop any wound issues, for example as oozy wound, redness, swelling around the wound site, or a high temperature please liaise with the ward you were discharged from. The nursing staff will provide you with more information about wound care on discharge.
Driving and work
You should not drive or work following your surgery. This is usually for 6 weeks until you come back to your clinic appointment and are seen by one of the consultants.
Leisure and sport
You will not be allowed to complete any form of leisure or sporting activities for around six months following your surgery. Your consultant or physiotherapist on the ward can advise you further on this.
Important contact numbers
- Whitney Dalby Advanced Clinical Practitioner in Spines – 07767 215241 /
This email address is being protected from spambots. You need JavaScript enabled to view it. - Helen Walton, Clinical Nurse Specialist in Spines - 07584 342593 /
This email address is being protected from spambots. You need JavaScript enabled to view it. - Physiotherapy Department - 0121 812 3500 (8am - 4pm, Monday to Friday)
Useful websites
- British Association of Spine Surgeons: spinesurgeons.ac.uk