Dupuytren's Disease
What is Dupuytren's Disease?
Dupuytren’s disease is a condition where the layer just beneath the skin, in the palm and fingers, thickens causing lumps (nodules), dints (pits) and cord like structures in the hand.
It does not affect the tendons which move the finger. It restricts the straightening by tightening up the palm side of the finger and hand.
The speed of progression of the disease and severity is very variable however when it progresses the tightening of the disease leads to the fingers curling into the palm. This most commonly affects the little and ring fingers.
The decision to have treatment for the disease is up to you and will usually depend on the level of inconvenience the condition causes.

Dupuytren's Contracture affecting the ring and small fingers.

Sever Contracture.
What causes Dupuytren's Disease?
The cause of the disease is not fully understood. The condition usually runs in families and is much more common in men than women. The disease has been associated with diabetes, alcohol use, liver disease and smoking however most patients have no clear cause for their contractures.
What treatments are available?
Needle Fasciotomy
This uses a needle to cut the cord to release the finger. The procedure is very simple and leaves very little scar. It is more commonly used in the palm than the fingers. This treatment has a much higher chance of the disease recurring than other treatment options but has a very quick recovery.
Fasciectomy
This is the surgical release of the finger where you will go to theatre and have the Dupuytren’s cut out of the hand, the skin is then stitched and a bandage, and sometimes a plaster cast is also applied.
Dermofasciectomy
This is a surgical removal of the Dupuytren’s in which a skin graft is taken from your arm or hip. This graft is stitched into the palm to replace poor quality skin or fill the gap in skin left when a very bent finger is operated on.
Treatment for Dupuytren’s will straighten your finger, often fully but the condition can be cured and may return. Treatment can improve your hands function. Treatment is usually safe but complications can happen.
What are the benefits of treatment?
The aim of treatment is to allow straightening of the fingers. If the finger is very curled it may not always be possible to achieve a fully straight finger with treatment. If a surgical option is chosen then the lumps (nodules) are also removed from the hand. No treatments are available to cure the disease and there is always a chance of the condition recurring.
After most procedures for Dupuytren’s you will see the hand therapists to help move your fingers and provide you with a splint to wear at night time in the post-operative period.
What happens on the day of treatment?
Admission
On the day of surgery, you will be admitted by a nurse who will check your details, medications and past medical conditions and put a wrist band with your details on the arm we are not operating on (if we are operating on both hands this band is put on your ankle). You will also be seen by an anaesthetist and a member of the surgical team before your procedure to go over any questions you may have, consent and to draw a mark on the arm you are having the operation on.
Remove any rings before you come to hospital and if you are unwell or have any cuts on your hand or arm then please inform us before the day as this may require your operation to be delayed.
Anaesthetic
Depending on what anaesthetic you have, you may have to starve for your surgery. You will be advised before your admission whether you will have to starve or not.
If you are having a general or axillary block anaesthetic you will be seen by the anaesthetist who will check your current health, ask specific questions about medications and when you have last eaten or drank.
If you are having a local anaesthetic, the surgeon will inject anaesthetic into your hand and if required a tourniquet will be put on your arm. This is to stop the blood flow in the arm while the operation is taking place. It is a tight band around the top of your arm similar to having your blood pressure taken.
If you are having an axillary block or general anaesthetic, the anaesthetist performs the anaesthetic. An axillary block will take 20-30 minutes to work, the anaesthetist and surgeon will check the arm is fully numb before surgery.
If you are staying awake for your surgery, there is the option to listen to music or watch a video on the tablet screens and headphones we have in theatre. Alternatively, you can bring your own device to listen to music on, but you must have headphones.
Surgery
Surgery time varies from 20-120 mins depending on the complexity of the Dupuytren’s disease and your surgeon will be able to tell you about the rough operative time on the day of surgery.
After surgery
You may go back to ADCU straightaway or sometimes sent to the recovery for one hour if you have had a general anaesthetic.
Once you are back in ADCU the nurses will make sure that you are sufficiently recovered from the operation before you are allowed home. You should have someone to take you home and be with you overnight after the operation.
Almost all patients will go home on the day of surgery. Very occasional, social or medical conditions require an overnight stay.
What complications can happen?
Overall significant complications are rare in Dupuytren’s surgery however the more severe the disease and the more procedures have taken place before on the finger, the increased likelihood of a complication.
The % values given cover a range from simple to complex cases. There are risks with the anaesthesia and your anaesthetist will discuss them with you.
Possible complications:
- Pain – the more extensive the surgery the more pain may be experienced, and this can occasional last longer than anticipated. If we feel pain killers will be required, they will be given to you on the day to take home.
- Scars may be tender for a number of months in 17% of patients.
- Chronic regional pain syndrome – this is a condition which is rare but can happen in 5-10% of patients with more extensive surgery. This condition is where there is increased pain and stiffness in the hand which may last many months and is treated with pain killers and physiotherapy.
- Bleeding – most wounds ooze a little and the dressing will usually soak this up and be fine until you are seen in a dressing clinic. Rarely (1-8%) there is increased bleeding which may soak the dressings. In this case please urgently contact the hospital and return for a change of dressing and review.
- Infection – infections occur in 2-7% of cases although it is extremely rare to need further surgery. A course of antibiotics will normally cure the infection. The wound will be reviewed in the dressing clinic after surgery to assess for any healing issues or any infection.
- Nerve injury – this can be cutting or bruising of the nerve which leads to a temporary or permanent loss of sensation in half or all of the finger. Again, this is rare in a primary procedure but occurs more frequently the more operations have taken place on the finger. (Nerve injury 3-27%, tingling or numbness 14%). There is also a possibility of nerve injury if having an axillary block. Temporary tingling or numbness occur in 1 in 100 patients with permanent problems in 1 in 3000 patients.
- Artery injury – this occurs in 2-31% of cases and, like nerve injury, increases the more surgeries take place. As there are 2 arteries in the finger it is very rare to lead to amputation of the finger but can lead to the finger being sensitive or painful or aching in cold weather (7% of cases).
- Stiffness – the stiffness will depend on whether the surgery was extensive and in many severe contractures the finger is not able to be fully straightened with surgery. Stiffness 4-15%
- Wound breakdown – wounds can breakdown or have delayed healing in 5-23% of patients. This usually just delays recovery but can occasionally lead to some permanent stiffness.
- Loss of skin graft – if you need a skin graft during surgery this may fail in 10-13% of patients. Usually the wound will then heal with just dressings, however occasional repeat surgery will be required. In 9% of patients the skin graft may contract causing some stiffness.
- Scar thickening – in 10% of patients the scar is a little thickened and in 9% the scar can contract and feel tighter in the palm.
- Tendon issues – in complex cases the tendon/rope that moves the finger may be cut (less than 1%) and in 3% of cases the tendon may become inflamed and sore for a few months making recovery slower.
- Amputation of finger – this will only really occur in complex revision cases or as a planned procedure due to poor function or a very severe contracture (1-3%).
- New problems - occasionally surgery on the hand, if extensive, can cause other problems such as carpal tunnel syndrome (6%), trigger finger (5%) and a swan neck deformity (abnormal bending of the finger 7%).
- Hair growth – in cases where a skin graft is taken, this often leads to hair growing on the graft site as it would normally do from where the skin was taken.
- Recurrence of contracture - this varies depending on which finger joint was involved, how straight the finger was after surgery and the type of surgery that took place. In general after 5 years the recurrence rates are 85% for needle fasciotomy, 25% for fasciectomy and 10% for dermofasciectomy. However not all patients who recur need or want further intervention.
What should I do about my medication?
Let the doctor know about your medication in the clinic. For all procedures other than local anaesthetic procedures you will be seen in the preassessment clinic before surgery who will advise exactly what to do regarding any medications which you will need to reduce or stop.
What can I do to make the operation a success?
- If you smoke it is best to stop or reduce as much as you can. If you are diabetic, you will reduce your risk of infection and poor wound healing by keeping your blood sugars stable.
- Attend all dressing, doctor and hand therapy appointments after surgery and follow instructions on hand exercises to get the best function and recover following surgery.
What happens after my surgery?
- You will go home on the same day and return to a dressing clinic, usually within a week, to assess your wounds and remove the plaster if present.
- You will have a splint applied and start exercises with the hand therapist if required. The appointments after this will depend on your recovery at the initial review.
- You can drive when your wounds are healed, and you feel you can safely grip the steering wheel in both hands to control the car.
- You can shower or bath as normal once the wounds are healed, but prior to that you need to keep the hand dry.
- Once fully recovered you will be discharged if no other fingers are causing issues. If you are part of a trial, additional appointments may be required however you will be clearly notified of this.
As Dupuytren’s is not curable there is always a chance it may return in the finger operated or appear in other fingers or the other hand. If this is the case, you would need to see your GP to be rereferred.
How quickly will I recover from the surgery?
Needle Fasciectomy
The wound will be reviewed at 1 week and usually by 2 weeks the hand is fully functional.
Fasciectomy
For open surgery the wound takes 2-3 weeks to heal and then it takes another 2-4 week to overcome the post-operative stiffness in most cases. In total, more severe cases can take 2-3 months to recover fully.
Dermofasciectomy
The skin graft is protected for 2 weeks with no movement to allow it to heal. Following this, the healing is similar to opened surgery. As grafts are usually used in more severe cases it is likely that recovery will take around 3 months.
In all these cases the flexibility and strength may improve after these timeframes but the majority of recovery and time to return to work is as detailed above.
During this recovery period you will see the doctor and the hand therapist in clinic. The hand therapist will make and adjust your hand splint if you need one and advise you on your progress and the exercises to undertake.
What happens if I don't get treatment?
Dupuytren’s does not get better by itself. The rate at which it worsens is very unpredictable. Although you do not have to have treatment you should be aware that the more curled up your fingers are the less likely it is to get them fully straight after treatment. In very severe diseases some patients may choose to have their finger amputated.
After surgery information
- Elevate your hand in a sling whilst mobilising and on a pillow when sitting or in bed.
- Do not allow your hand to hang down by your side.
- Keep the dressing dry, try not to disturb the dressing until you have been advised to.
- Do not partake in heavy manual work until you have been seen at your next appointment and have been advised it is safe to do so.
- Take painkillers as prescribed.
- If you are instructed to wear a sling, please ensure you remove your arm from the sling every 1 to 2 hours and exercise the shoulder and elbow to prevent them from getting stiff. Remember to also wriggle your fingers.
If you experience pain, numbness, tingling, excessive swelling, discharge through your dressing or discoloration of the fingers, in the first instance please contact the Outpatients Department (Mon - Fri, 8:30am - 4:30pm).
Outside of these hours, please contact the main hospital number and ask for the Clinical Site Co-Ordinator on call: 0121 685 4000.
If you are unable to make your Outpatient appointment, please contact the Appointments department on 0121 812 3200.
Post-operative exercises
Finger Exercises
Starting from a straight position, do 10 repetitions of each type of fist shown
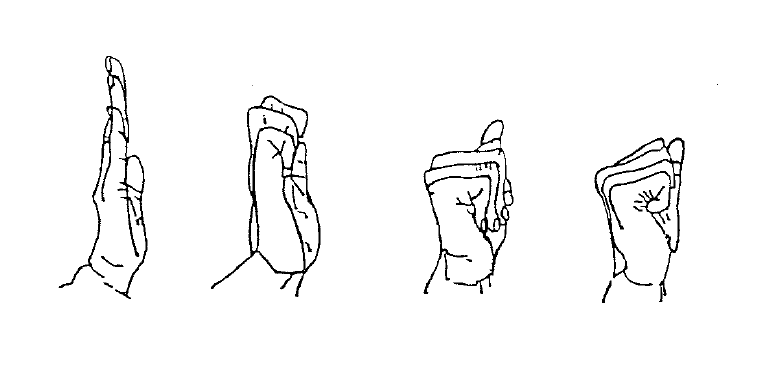
Therapy information